Even though menopause is a natural, biological process and something that half of the world’s population will experience in their lives, it still remains a taboo topic and one that many medical practitioners are not well-educated in or trained on how to manage. This lack of education and support leaves women in the dark about how to navigate this important stage of life, and often we end up suffering through uncomfortable and even debilitating symptoms that can also lead to an increased risk of numerous chronic illnesses.
Since our bodies go through significant changes during this phase, which can begin as early as our mid-30s, it is incredibly important to understand exactly what is happening as you go through perimenopause, and ultimately reach menopause. We shouldn’t be expected to simply endure these symptoms – we deserve to feel great and live our lives to the fullest. With that in mind, let’s dive into the four stages of menopause, some of the symptoms that can be expected, how the loss of our hormones affects our long-term disease risk, and tips to help navigate this transition better and feel our best!
Did You Know Menopause Is Only One Day?
Menopause is defined as the one-year anniversary of the last day of your final period. The term menopause is often used to describe the entire phase of the menopausal transition years, but in actuality, you are only “in” menopause for that one day when it has been a full year without menstrual bleeding. Every year before this day, you are actually going through perimenopause.
What Are the Four Stages of Menopause?
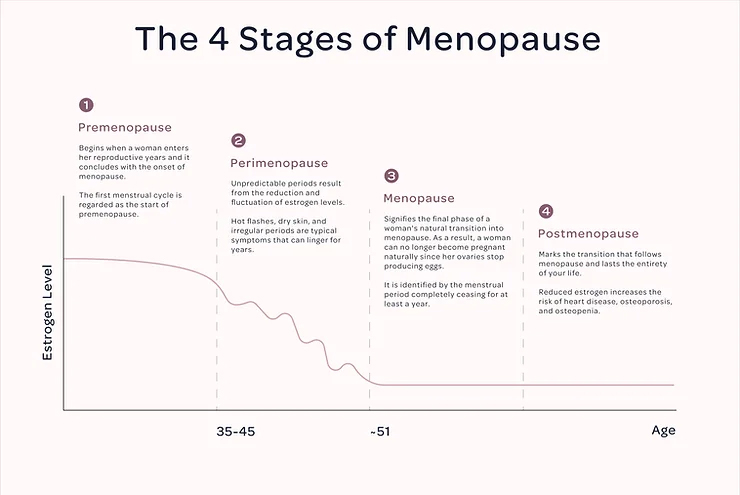
There are four stages of menopause, each of which have their own symptoms, hormone levels, and age range/duration. The four stages are:
● Premenopause
● Perimenopause
● Menopause
● Postmenopause
Here’s a deeper look at what you can expect during each of these four stages:
Premenopause Stage
As its name suggests, the premenopause stage begins with the first menstruation during puberty and ends with perimenopause when the female hormones, estrogen and progesterone, begin to fluctuate and diminish. During this stage, a woman has her regular menstrual cycle and no noticeable symptoms of perimenopause.
Most women will begin this stage during their pre-teen or early teen years until perimenopause begins.
Perimenopause Stage
Perimenopause is the time when estrogen and progesterone levels begin to fluctuate and drop, which can begin as early as the mid-30s. The loss of these hormones leads to over 50 potential symptoms, some of which can be quite debilitating. Some of these symptoms are well-known, such as hot flashes, hair loss, and weight gain, however, there are many lesser-known symptoms associated with perimenopause, such as tinnitus, heart palpitations, and mood disorders. So many of these symptoms are often undiagnosed, untreated, or treated as separate diagnoses rather than one single condition. As a result, many women are not offered proper care and continue to suffer.
Menopause Stage
Menopause occurs when you have gone without a period for 12 consecutive months. As such, women “experience” menopause only on that one day in their life.
Menopause usually occurs for most women sometime between their mid-40s and mid-50s, but this varies from person to person. The average age of menopause for a woman in the United States is 51 years old. Many perimenopausal symptoms will diminish or disappear after menopause has occurred and the body adjusts to the absence of female hormones. However, for some women, the symptoms of perimenopause may continue even after menopause.
Postmenopause Stage
Postmenopause takes place after you have surpassed a full year without a menstrual cycle and menopause has occurred. This stage lasts for the rest of your life.
During this time, many of the symptoms that are associated with perimenopause have disappeared, or gradually decrease. However, due to lower levels of hormones like estrogen, postmenopausal women are at an increased risk for various health conditions, including:
● Osteoporosis
● Cardiovascular disease
● Vaginal atrophy
● Dementia
● Urinary tract infections (UTIs)
How to Address Perimenopausal Symptoms
Here are some tips to not only help alleviate some of the most common symptoms of perimenopause, but also reduce your risk of long-term disease:
● Diet: During this time, women do not process sugars effectively, putting them at risk of glucose intolerance and diabetes. Lower levels of estrogen also contribute to increased levels of bad cholesterol (LDL) and triglycerides. Therefore, a whole foods diet focuses on a variety of vegetables, low glycemic fruits, unprocessed whole grains, organic free-range chicken/ eggs, grass-fed beef, and sustainably sourced low-mercury fish. Eating this way can also help reduce some of the common symptoms experienced during perimenopause such as hot flashes, brain fog, fatigue, and acid reflux.
● Exercise: Lower levels of estrogen contributes to a reduction in bone density, and increased risk of osteoporosis. As testosterone levels drop, maintaining muscle mass becomes increasingly difficult. Incorporating daily low-impact exercise can be beneficial, such as brisk walks, swimming, cycling, or yoga, and strength training 2–3 times weekly to maintain bone density and muscle mass. Regular exercise can also aid with improving mental health, weight gain, and low energy.
● Sleep: Perimenopause has a significant impact on sleep. Insufficient or poor-quality sleep has been shown to have a negative impact on long-term health and may be one of the risk factors for developing dementia. Poor sleep also leads to chronic fatigue and brain fog. Thus, women must focus on improving sleep hygiene. Consider using an eye mask, white noise machine, disconnecting from devices at least one hour before bedtime, and maintaining a regular sleep/wake schedule to help achieve at least 7 hours of quality sleep each night. Some supplements that might also be beneficial are magnesium glycinate, L-theanine, and melatonin.
● Stress reduction: Lower levels of estrogen lead to increased levels of cortisol, the stress hormone, in our bodies. This leads to numerous mood disorders in perimenopausal women, such as anxiety, depression, feelings of rage, and irritability. Focusing on reducing stress with journaling, meditation, breath work, or spending time in nature can be very beneficial. Supplements containing adaptogens (ashwagandha, rhodiola, chaga, holy basil) can help the body cope with these increased levels of stress.
● Gut health: Fluctuating hormones impact the health of our gut microbiome. As such, avoiding foods and environmental toxins that contribute to inflammation in our bodies is essential. Try to buy organic produce whenever possible, and reduce or eliminate pre-packaged foods, alcohol, refined carbohydrates, and processed meats. Incorporating probiotic foods, such as kimchi or sauerkraut, or taking a probiotic supplement can help repopulate the good bacteria in our gut.
● Hormone Replacement Therapy (HRT): Newer forms of HRT have been shown to have a significant impact on reducing or eliminating the symptoms of perimenopause, as well as, reducing the risk of several chronic diseases that affect women during this time. Recent evidence shows that these newer formulations (topical estradiol and oral micronized progesterone) do not, in fact, increase the risk of breast cancer or blood clots. This is an option that really should be offered to all women who can safely use HRT, so they may make an informed decision on not only improving their current symptoms but also protecting their long-term well-being.
To learn more about perimenopause and other women’s health issues, be sure to read Dr. Kavita Desai’s new book, Lady Parts: Putting Women’s Health Back Into Women’s Hands, and follow her women’s health & wellness company, Revivele, on Instagram, Facebook, and LinkedIn!